What is atopic dermatitis and what you need to know.
1. What is atopic dermatitis?
Atopic dermatitis, also known as atopic dermatitis, is a skin disease caused by an overactive immune system. The disease is common in children and usually lasts a lifetime. Signs of atopic dermatitis is an itchy, red rash that may contain fluid. The disease is often accompanied by asthma, allergic rhinitis, urticaria, … For people with a family history of atopic dermatitis, the likelihood of the disease will be about 60%.
2. Signs and symptoms of atopic dermatitis
- Dry, thickened, scaly skin;
- Itchy;
- Erythema;
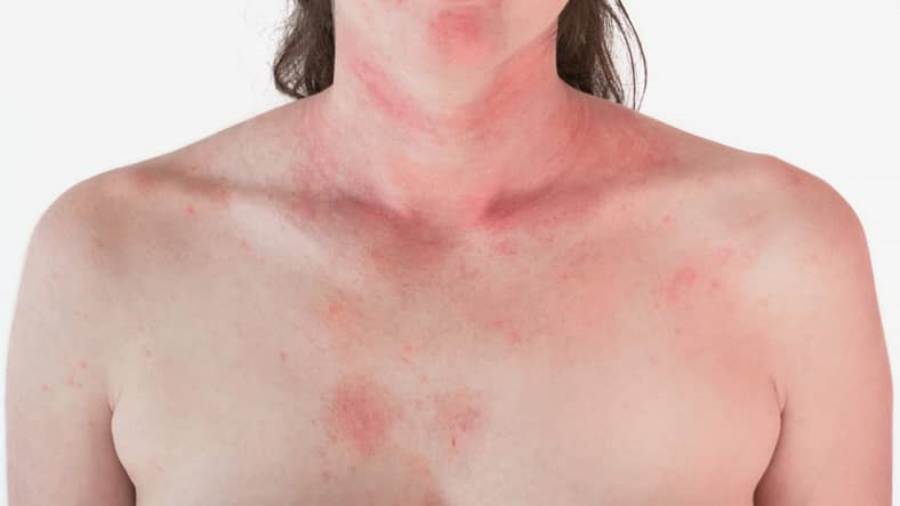
- Symptoms usually appear on the face, neck, chest, wrists, arms, back of the knees, and legs.
Atopic dermatitis in children and adults has similar manifestations. For children, the disease usually appears at the age of 2 – 3 months, or if it is slower, it can appear when the child is 2 years old. Symptoms of the disease are common in the neck, face and scalp. In the affected areas, there will be itching and flaking of the skin. If the child scratches, the skin will thicken and the child will show signs of insomnia.
For adults, when atopic dermatitis appears, it will cause a rash and persistent itching, which can occur on the whole body. The itching will get worse and worse if left untreated.
3. When you have to see a doctor?
In the case of scratching too much can cause superinfection of the skin leading to skin infection; causes red streaks, yellow scales, or pus to appear. In addition, atopic dermatitis can affect the eyesight of the eyes, reduce mental concentration, make the patient lose sleep and feel uncomfortable in daily activities or when communicating. So, when you notice signs of persistent itchy skin, or using common allergy medicine has not shown any signs of improvement, you should see a dermatologist for examination and treatment plan.
4. Causes of atopic dermatitis
The cause of atopic dermatitis is still unknown. Many studies show that this is a combination of genetic factors and some environmental factors such as stress, weather, exposure to allergens such as cement, rubber, chemicals, detergents, bacteria, parasites,…
5. Who is at risk for atopic dermatitis?
Atopic dermatitis is more common in infants and children. Some studies have shown that the incidence is higher in men than in women.
Factors that increase your risk of atopic dermatitis include:
- Heredity: If a parent has ever had atopic dermatitis or diseases with allergic factors such as asthma, allergic rhinitis, urticaria, etc., the child has a 60% chance of having the disease. In cases where both parents have a history of the disease, the chance of the child developing the disease increases to 80%.
- People are constantly exposed to dirt, medical articles, chemicals, cleaning agents and other allergens.
- For children, living in a densely populated area, going to daycare, and having hyperactivity disorder (ADHD) increase the risk of atopic dermatitis.
6. Methods of diagnosis and treatment
6.1. Methods of testing and diagnosis of atopic dermatitis
Doctors diagnose atopic dermatitis by:
- Examine the skin and observe for manifestations on the skin and eyes.
- Take the medical history to determine if atopic dermatitis is familial or from other diseases with an allergic factor.
- Skin biopsy: A small sample of the skin is taken from the affected area for testing to rule out an infection.
6.2. Effective treatment for atopic dermatitis:
There is no definitive cure for atopic dermatitis. General principles of treatment include:
- Reduce skin symptoms such as dry skin, itchy skin, skin rash, thickened skin;
- Anti-infective, anti-inflammatory;
- Advise the patient and family on how to take care of the skin at home to prevent the disease from getting worse.
Treatment of atopic dermatitis requires a combination of medication, self-care, and lifestyle changes. Specific treatments are:
Use medicine:
+ Anti-itchy skin: H1 antihistamine, fexofenadin 180 mg, certerizine 10 mg. In severe cases, corticosteroids such as prednisone, diphenhydramine, and hydroxyzine may be used.
+ Anti-dry skin: Use 10% urea, petrolatum with dry skin.
+ Anti-scalding: 5% – 10% salicyle ointment, goudron grease, ichthyol, crysophanic.
+ Anti-infective: Use 1st generation cephalosporin antibiotics.
Depending on the patient’s condition and the severity of the disease, the doctor will prescribe the appropriate medication. You absolutely should not buy medicine and treat it at home without the guidance of a professional doctor.
Read more articles:
8 best nutrients and vitamins for healthy and strong nails
How chondroitin protects and strengthens cartilage
Effective herbs to improve concentration and increase energy production